Obesity: All You Need to Know
Obesity is a complex health condition that occurs when there’s an accumulation of excessive body fat. It’s characterized by an excess of adipose tissue, which can have negative effects on health.
It’s a global issue that poses significant health risks and has been linked to a number of chronic diseases such as diabetes, heart disease, and certain cancers.
Its prevalence has dramatically increased, with the World Health Organization (WHO) reporting in 2016 that more than 1.9 billion adults were overweight, and of these, over 650 million were classified as obese.
This piece aims to provide a comprehensive overview of obesity, exploring its causes, consequences, and potential solutions.

What is body mass index (BMI) and how do we define obesity?
The body mass index (BMI) is a calculation that considers both weight and height to assess body size. It is commonly used by medical professionals as a screening tool for obesity.
It’s important to note that BMI does not distinguish between muscle and fat mass, and therefore cannot be used as an accurate indicator of health.
Apart from BMI, growth charts are used to assess childhood obesity.
Types of Obesity
Healthcare providers categorize obesity into different classes based on its severity. They use BMI as a measurement. If your BMI falls between 25.0 and 29.9 kg/m², you would be classified as overweight. There are 3 general classes of obesit:
Class I obesity: BMI 30 to <35 kg/m².
Class II obesity: BMI 35 to <40 kg/m².
Class III obesity: BMI 40+ kg/m².
What is Childhood Obesity?
Childhood obesity is a serious medical condition that occurs when children and adolescents are significantly above the average weight for their age and height.
Childhood obesity assessment is a crucial step in identifying and managing obesity early on. Medical practitioners typically use growth charts that account for a child’s age and gender to assess weight status. These charts plot a child’s Body Mass Index (BMI) percentile, with over the 95th percentile considered obese, between the 85th and 95th percentile deemed overweight, and less than the 85th percentile considered a healthy weight.
Morbid Obesity Class 3
Morbid obesity, also known as Class III obesity, is a severe form of obesity characterized by a body mass index (BMI) of 40 or higher. It significantly increases the risk of obesity-related health conditions or co-morbidities, such as heart disease, diabetes, and certain types of cancer. These health risks can dramatically reduce life expectancy and impact quality of life. It’s important to remember that morbid obesity isn’t just about weight – it’s a serious health condition that requires medical intervention.
What are the causes of Obesity?
Obesity is a complex and multifactorial condition that is influenced by a variety of factors, including genetics, lifestyle choices, and environmental factors.
Caloric intake plays a significant role in weight gain. Eating more calories than the body burns off can lead to weight gain. Other factors that can contribute to obesity include physical inactivity, poor sleep habits, and certain medications.
Most Common Causes of Obesity:
- Poor Diet: Consuming high-calorie foods, particularly processed and fast foods, contributes significantly to obesity. These foods tend to be high in fats and sugars, leading to an excess caloric intake.
- Sedentary Lifestyle: Lack of physical activity is another major factor leading to obesity. Living a sedentary lifestyle leads to weight gain as it means burning fewer calories.
- Genetics: Genes play a role in how your body processes food into energy and how fat is stored. Genetic factors might also affect the amount of food you eat and your level of physical activity.
- Psychological Factors: Emotional issues such as stress, depression, and trauma can lead to obesity. Some people eat more than usual whenever they’re stressed or depressed.
- Medications: Some medications can lead to weight gain: corticosteroids, which may treat autoimmune disease, antidepressants, antipsychotics and beta-blockers, which may treat high blood pressure
- Medical conditions: Certain health conditions can also lead to weight gain, which may lead to obesity : hypothyroidism, polycystic ovary syndrome (PCOS), metabolic syndrome, Prader-Willi syndrome, and Cushing’s syndrome can cause obesity.
How to Diagnose Obesity?
Doctors diagnose obesity through medical history, physical examination, and laboratory testing.
Medical History: The doctor will ask about your health history and lifestyle habits to determine if you are at risk for obesity.
Physical Examination: Doctors measure height, weight ,and waist circumference to calculate body mass index (BMI). BMI is used to determine whether an individual has a healthy weight.
Laboratory Testing: Laboratory tests such as blood tests and urine tests may be ordered to evaluate health status and identify any medical conditions that could contribute to obesity.
What are the consequences of Obesity?
Obesity can have serious implications for an individual’s health and well-being. It increases the risk of developing chronic diseases.
The linking of obesity to numerous health conditions has been widely validated through extensive research. Some commonly associated diseases include:
- Heart Disease : Obesity is directly related to heart disease. Excess weight, specifically in the abdominal region, increases the strain on the heart and raises blood pressure and cholesterol levels, leading to coronary heart disease.
- Diabetes : Type 2 diabetes and obesity often go hand in hand. Obesity causes insulin resistance which leads to elevated blood sugar levels, ultimately resulting in diabetes.
- Cancer: The risk of several types of cancer, including breast, colon, kidney, and esophagus, increases with obesity. The exact correlation is still under investigation, but it may be due to systemic inflammation or hormonal changes caused by obesity.
- Sleep Apnea: Obesity, particularly abdominal obesity, is a significant risk factor for sleep apnea. The excess fat tissue can block the airway during sleep, causing irregular breathing patterns or shortness of breath.
- Mental Health Issues: Obesity impacts mental health as well. It can lead to depression, anxiety, low self-esteem, and other psychological disorders due to societal pressures and personal struggles with body image.
In addition to these health-related consequences, obesity also affects the quality of life and social interactions of the individuals. It can restrict physical activity, leading to difficulty in performing daily tasks and can induce social isolation.
How is Obesity Treated?
Your personalized treatment plan will be based on a comprehensive health profile. Your doctor will prioritize addressing your most pressing health concerns, followed by a long-term weight loss strategy.
Generally, they may recommend prompt changes, such as adjusting your medications, to bring about immediate impact. The overall treatment plan will progress gradually, taking into account various factors. Since each individual is unique, it may take some trial and error to identify the therapies that yield the best results for you.
Obesity is typically treated with lifestyle changes, including a healthy diet and regular exercise. However, this approach does not always lead to sustained weight management. In some cases, medications or surgery may be needed.
Medications for Obesity
Certain medications can be prescribed to assist in managing obesity when lifestyle modifications alone prove ineffective. These medications may include anticonvulsants, antidepressants, and other drugs.
It’s worth noting that medications alone are not a complete solution for weight loss, but they do present an alternative approach. For example, appetite suppressants can intercept specific pathways to the brain that influence hunger. While this may offer a partial solution for some, it can play a more substantial role in the weight loss journey for others. Remember, choosing the right medications can be a key component in achieving successful weight loss.
Common FDA-approved drugs for treating obesity include:
Phentermine (Adipex-P®, Lomaira®, Suprenza®): Decreases appetite. Approved for three-month use.
Benzphetamine (Didrex®, Regimex®): Suppresses appetite.
Diethylpropion (Depletite # 2®, Radtue®, Tenuate®): Reduces appetite.
Phendimetrazine (Bontril®, Melfiat®): Suppresses appetite.
Liraglutide (Saxenda®): Reduces appetite and slows digestion.
Semaglutide (Wegovy®): Suppresses appetite.
Cellulose and citric acid (Plenity®): Provides a feeling of fullness.
Phentermine-topiramate (Qsymia®): Reduces hunger.
Weight-Loss Surgery (Bariatric Surgery) for Obesity
When it comes to treating obesity, bariatric surgery can be an effective method, particularly when other options have failed. There are several types of weight-loss surgeries, each with their own pros and cons, and the best option depends on the individual’s specific circumstances.
- Gastric Bypass (Roux-en-Y Gastric Bypass): This is the most common type of bariatric surgery. It works by bypassing a large part of the stomach and creating a smaller pouch. This surgery not only restricts the amount of food you can eat but also the amount of calories your body can absorb.
- Adjustable Gastric Banding (Lap-band Surgery): In this surgery, a band is placed around the upper part of the stomach to create a small pouch. The band can be adjusted to control the size of the opening to the rest of the stomach, controlling the amount of food it can hold.
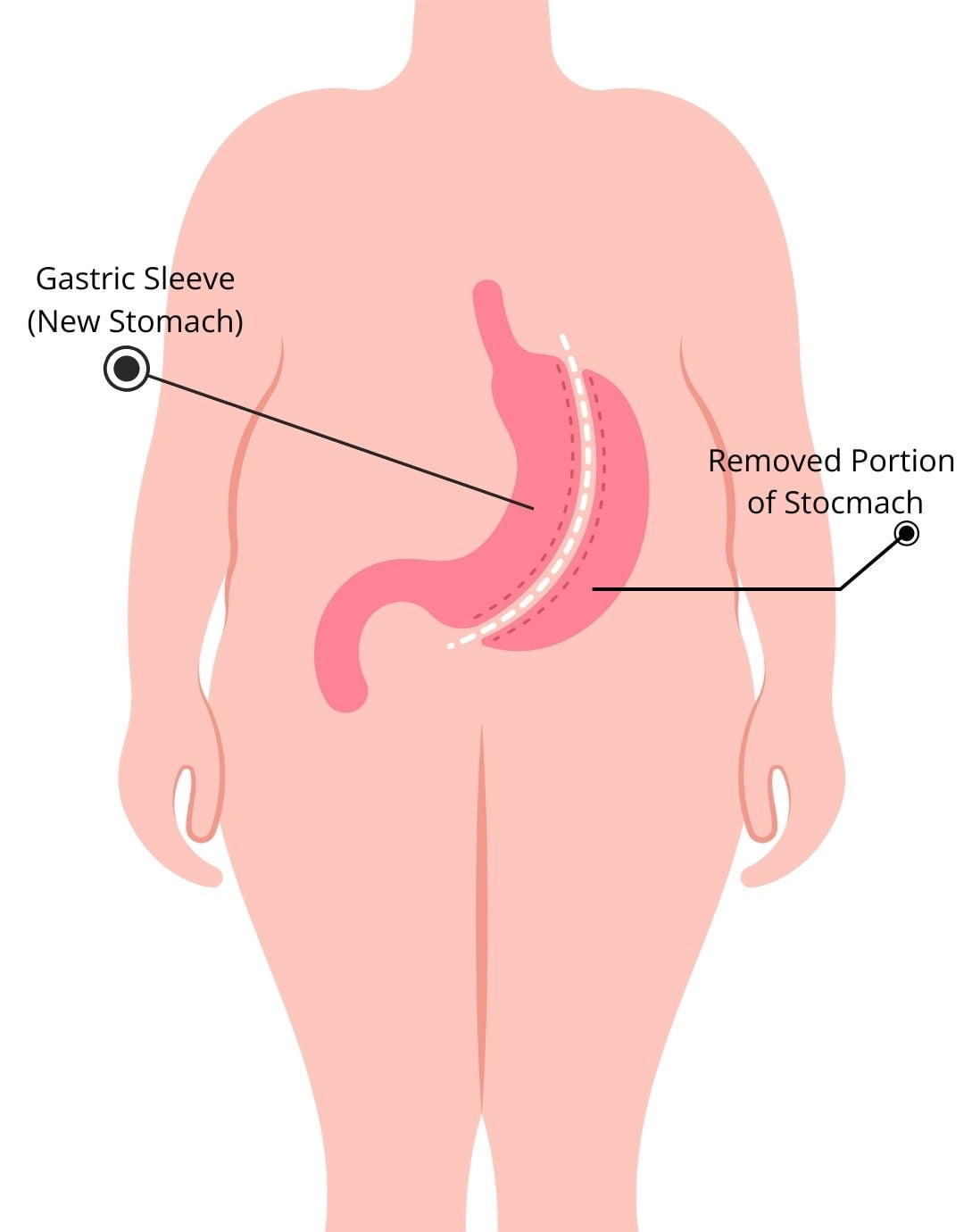
- Sleeve Gastrectomy: This procedure removes about 80% of the stomach, leaving a long, tube-like structure. It promotes weight loss by restricting the amount of food that can be eaten, without interfering with the absorption of nutrients.
- Biliopancreatic Diversion with Duodenal Switch (BPD/DS): This is a more complex type of surgery that involves removing a large part of the stomach and bypassing a significant part of the small intestine. This surgery can lead to significant weight loss but also has more potential complications.
Candidacy on Weight Loss Surgery:
Candidates for weight loss surgery typically have a body mass index (BMI) of 40 or higher, or a BMI of 35 or higher along with serious weight-related health issues, such as type 2 diabetes, high blood pressure, or severe sleep apnea. In some cases, individuals with a BMI of 30 to 34 with serious health problems related to obesity may qualify for certain types of weight-loss surgery.
It’s important to note that surgery is generally viewed as a last resort after all other methods of weight loss, including lifestyle changes and medications, have been tried without success. Furthermore, it’s crucial to understand that while bariatric surgery can help contribute to weight loss, continued lifestyle changes are necessary to maintain long-term weight loss post-surgery.
Non Surgical Options to Treat Obesity
Non-surgical weight loss procedures may also be considered for those looking to improve their overall health and well-being. These include lifestyle intervention programs that focus on nutrition and exercise, as well as various noninvasive technologies such as:
- Gastric Balloon: This non-surgical procedure involves placing a balloon in the stomach to reduce the amount of food it can hold, thus creating a feeling of fullness even after eating small amounts of food.
- Swallowable Gastric Balloon: The swallowable gastric balloon procedure involves swallowing a capsule tied to a thin tube. Once the capsule reaches the stomach, it’s filled with a sterile solution to take up space in the stomach and encourage smaller meal portions.
- AspireAssist: AspireAssist involves the use of a tube to drain a portion of the stomach’s contents after each meal. This helps in reducing the amount of calories absorbed by the body, aiding weight loss.
- Vagal Blocking (vBloc Therapy): vBloc Therapy utilizes a pacemaker-like device that is implanted under the skin. This device sends intermittent electrical pulses to the abdominal vagus nerve, which tells the brain when the stomach feels empty or full.
- Gastric Botox: This technique involves injecting Botox into the stomach walls to slow down digestion and increase feelings of fullness. This can help reduce portion sizes and encourage weight loss.
How to Prevent Obesity?
Lifestyle and Dietary Changes for Obesity Prevention
Adopting a healthy lifestyle is the cornerstone of obesity treatment. Here’s what that might entail:
- Dedicate Regular Time for Physical Activity: Engage in at least 150 minutes of moderate aerobic activity or 75 minutes of vigorous activity each week, along with strength training exercises twice a week. This can help burn excess calories and improve metabolism.
- Adopt a Balanced Diet: Incorporate a variety of nutrient-rich foods from all food groups into your meals. Limit the intake of processed foods, sugars, and unhealthy fats.
- Mindful Eating: Pay attention to what and when you eat. Try to eat at regular intervals and avoid skipping meals.
- Portion Control: Avoid oversized portions, especially when eating out. Start with smaller amounts and decide if you’re truly still hungry before going back for more.
- Limit Alcohol: Alcohol can add excess calories to your diet and increase your risk of weight gain.
- Get Adequate Sleep: Lack of sleep can interfere with your body’s hunger hormones and lead to weight gain.
- Manage Stress: Stress can lead to overeating or unhealthy food choices. Find healthy ways to cope with stress, such as physical activity, meditation, or talking to a mental health professional.
Last Words from the More CLinics
Obesity management involves a multifaceted approach, including lifestyle modifications, medications, and in severe cases, surgical intervention. Bariatric surgeries offer effective solutions when other methods prove insufficient. However, these are typically considered as a last resort and require a commitment to lifestyle changes post-surgery for successful long-term weight maintenance.
The More Clinics Turkey is offering a variety of medical and dental treatments since many years. With the help of our experienced medical team, you can find the right solution for your unique situation, giving you back your confidence and self-esteem. Contact us today to learn more and get your Free Consultation.
GET A FREE CONSULTATION!
Let’s Start Planning Your Treatment %100 Guarantee Results.