Retinal Detachment Causes & Symptoms & Treatment
Retinal detachment is a serious and emergency eye condition that demands immediate attention. It occurs when the retina, a thin layer of tissue that lines the back of the eye, is pulled or lifted away from its normal position. This can lead to vision loss or blindness if not treated promptly. In this guide, we will delve into the retinal detachment symptoms and causes, as well as discuss risk factors and available treatment options, with valuable insights from The More Clinics.
What Is Detached Retina?
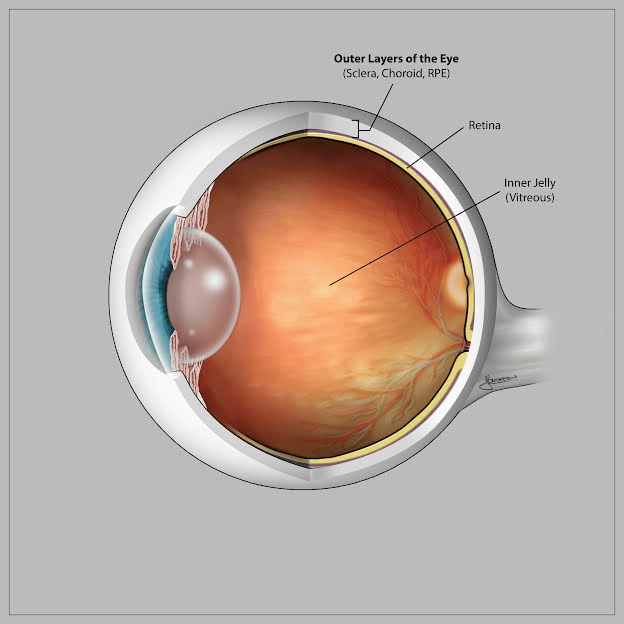
A detached retina is a serious condition where the retina — the layer of tissue at the back of the eye that processes light and color — peels away from the underlying tissue to which it’s attached.
The detachment causes the retinal cells to separate from the layer of blood vessels that provides oxygen and nourishment, resulting in the malfunction of this sensory equipment. The impacted areas lose their ability to respond to incoming light signals, which can result in vision loss.
It’s crucial to seek immediate medical attention if you notice any signs of retinal detachment, as it is considered an ocular emergency.
Retinal Detachment Types
Retinal detachment isn’t a one-size-fits-all condition. There are three main types: rhegmatogenous, tractional, and exudative.
Rhegmatogenous retinal detachment : this is the most common type of detachment that occurs when a tear or hole forms in the retina. This occurrence allows fluid to seep beneath the retina, causing it to separate from the underlying tissue. Typically associated with aging, this condition arises as the vitreous gel inside the eye becomes more watery, leading to its shrinkage or detachment from the retina.
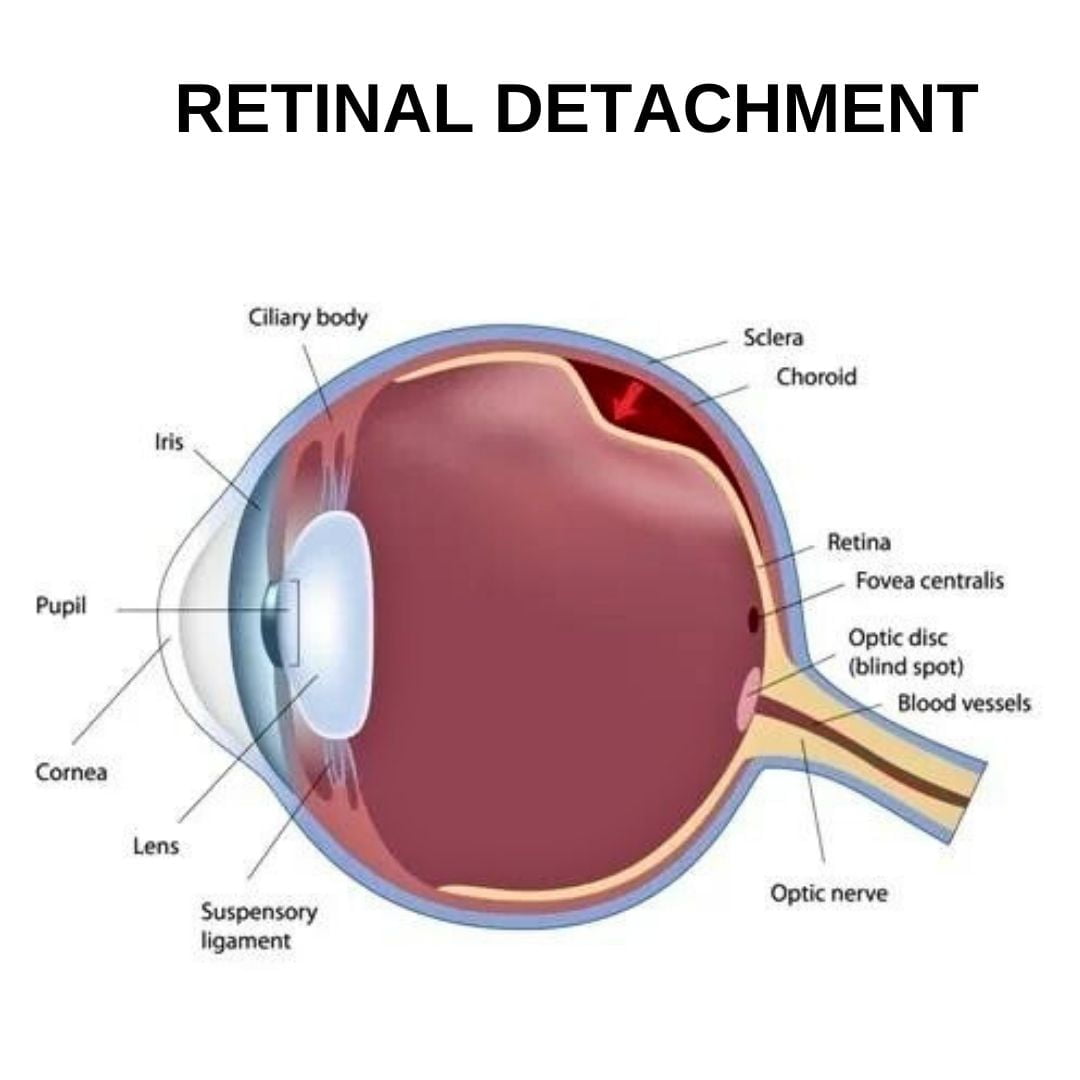
Tractional retinal detachment: this type of detachment occurs when scar tissue forms on the surface of the retina and pulls it away from its normal position. This condition is typically observed in individuals who have diabetes, as it causes damage to the blood vessels located at the posterior of the eye.
Exudative retinal detachment: this type of detachment is caused by the accumulation of fluid beneath the retina, which can be due to inflammatory disorders, injury, or certain types of eye tumors.
Retinal Detachment Symptoms
The retinal detachment symptoms can appear suddenly and may include:
- Floaters: These are small specks or clouds that float in your field of vision. They can appear suddenly and may increase in number.
- Flashes of light: You may start seeing flashes of light, especially in peripheral (side) vision.
- Blurred vision: There could be a gradual or sudden decrease in your vision clarity.
- Darkening vision or shadow: You might perceive a curtain-like shadow moving across your field of vision, typically from the periphery towards the center.
- Loss of vision: In severe cases, there might be a sudden and significant loss of vision. This could be described as a “blackout.”
It’s essential to seek medical attention immediately if you experience any of these retinal detachment symptoms.
Risk Factors
Certain factors can increase your risk of developing retinal detachment, including:
- Age: The risk increases with age, especially after 40 years.
- Previous retinal detachment: If you have had a retinal detachment in one eye, you are at a higher risk of developing it in the other eye.
- Family history: If you have a family history of retinal detachment, your risk is elevated.
- Nearsightedness: Individuals with severe nearsightedness (myopia) have higher chances of developing this condition.
- Eye surgery or injury: Previous eye surgeries, such as cataract removal, and eye injuries can increase the risk of retinal detachment.
- Other eye conditions: Conditions such as lattice degeneration or other structural abnormalities in the retina can also put you at a higher risk.
Diagnose & Treatment
How is it Diagnosed?
A detached retina can be diagnosed through a comprehensive eye exam, which may include the following procedures:
- Dilated Eye Exam: The pupil is widened with eye drops to allow a closer look at the retina. The doctor uses an ophthalmoscope, a tool that shines a bright light into the eye and magnifies the retina, allowing for a clear view of any retinal detachment.
- Ultrasound Imaging: If bleeding has occurred in the eye, making it cloudy and hard to see the retina, an ultrasound might be used. This test uses sound waves to visualize the retina, helping the doctor to see whether it’s detached.
- Optical Coherence Tomography (OCT) or Computed Tomography (CT): These tests provide high-resolution images of the retina and can help detect any changes in its structure.
Retinal Detachment Treatment
This eye condition is a medical emergency that requires prompt treatment to prevent permanent vision loss. Depending on the type and severity of the detachment, your doctor may recommend one of the following treatments:
- Laser surgery (photocoagulation): This procedure involves using a laser to form burns around the tear or hole in the retina, creating scar tissue that seals the area and prevents further fluid leakage.
- Cryopexy(freezing): In this procedure, extreme cold is used to freeze the area around the retinal tear or hole, creating a scar that helps seal it.
- Scleral buckling: This surgery involves placing a silicone band around the eye to push the wall of the eye against the detached retina. This positioning helps seal any holes, openings or breaks in it.
- Vitrectomy: During this surgery, your doctor removes the vitreous gel from the eye and replaces it with saline solution (a mixture of water and salt), which helps reattach the retina.
- Pneumatic (gas bubble) retinopexy: This procedure involves injecting a small gas bubble into the vitreous cavity of the eye. The bubble expands and pushes against the detached retina, helping to reattach it.
In some cases, a combination of these treatments may be necessary to successfully repair the detached retina. After treatment, regular check-ups are necessary to monitor your vision and ensure that the retina remains attached. With timely diagnosis and appropriate treatment, retinal detachment can be successfully treated in the majority of cases.
How To Prevent?
While some risk factors, such as age and family history, can’t be controlled, there are steps you can take to reduce your chances of developing retinal detachment:
- Have regular eye exams: Regular eye check-ups can help detect any signs of retinal detachment early on, allowing for prompt treatment.
- Manage chronic health conditions: If you have diabetes or hypertension, it’s essential to keep them under control to reduce your risk.
- Protect your eyes during physical activities: Wear protective eyewear when participating in sports or activities that could result in eye injuries.
- Avoid smoking: Smoking can increase your risk of developing retinal detachment, so it’s best to avoid it altogether.
- Be aware of changes in vision: It’s crucial to be aware of any changes in your vision and seek medical attention if you experience any symptoms.
Frequently Asked Questions
Yes, some cases may have subtle or no warning signs. Regular eye check-ups are crucial for early detection.
Not necessarily. While pain may not always be present, sudden flashes of light and floaters are common symptoms.
Yes, it is possible to experience a detached retina multiple times. This is why regular eye exams and monitoring by your doctor are important even after successful treatment of a detached retina. If you notice any changes in your vision or symptoms returning, contact your doctor immediately for further evaluation and treatment. Keeping up with preventative measures can also help reduce the risk of repeat detachments.
You should seek immediate medical attention by going to the emergency room if you experience sudden changes in your vision. Symptoms such as an increase in the number of floaters, sudden flashes of light in one or both eyes, a shadow or curtain over a portion of your visual field, or a sudden decrease in vision indicate an urgent need for medical evaluation as they could be signs of detachment or other serious eye conditions.
Retinal detachment is relatively rare, affecting about one in 10,000 people each year. However, the incidence increases with age, especially in individuals over the age of 40. Additionally, the condition is more common in men than in women, and in people who are severely nearsighted. You can learn more about this through the National Eye Institute’s page.
Yes, trauma to the eye or head can lead to retinal detachment. Seek immediate medical attention after any injury involving the eyes.
Maintaining overall eye health, avoiding smoking, and protecting your eyes from injury can contribute to preventing retinal detachment.
Success rates vary, but early detection and prompt treatment significantly improve the chances of successful surgery.
Yes, aging increases the risk of retinal detachment. Regular eye check-ups become even more crucial as you age.
Last Words from The More Clinics
Retinal detachment is a serious condition that can cause permanent vision loss if not treated promptly. Those over 40, with a family history, severe nearsightedness, previous eye surgeries, or certain eye conditions are at higher risk. Regular eye exams, managing chronic conditions, eye protection during activities, not smoking, and being aware of vision changes can help prevent it. Seek immediate medical attention if you experience symptoms like floaters, flashes of light, blurred vision, or vision loss.
Remember, your eyesight is precious. Don’t delay – schedule your eye exam with us today at The More Clinics. Early detection and treatment are key to preserving your vision. We’re here to help you every step of the way. Contact us now!
GET A FREE CONSULTATION!
Let’s Start Planning Your Treatment %100 Guarantee Results.








